Imaging, QoL and Patient-Reported Outcome and Supportive Care
Daratumumab treatment in the patients’ own home.
P-132: Daratumumab treatment in the patients’ own home.
Wednesday, September 25, 2024

Thomas Lund, MD, PhD (he/him/his)
Associated Professor
Department of Hematology Odense University Hospital, Syddanmark, Denmark
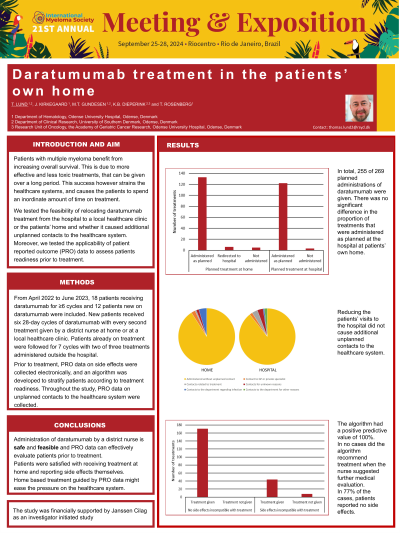
Introduction: Patients with multiple myeloma benefit from increasing overall survival. This is due to more effective and less toxic treatments that can be given for a long time. The success however strains the healthcare system and causes the patients to use substantial time on treatment. We tested if part of the treatment could be given outside the hospital, and if electronic Patient Reported Outcome (PRO) data could determine if patients needed to talk to a healthcare practitioner before each injection.
Methods: From April 2022 to June 2023, 30 patient were included, mean age was 76; range 61-87. Eighteen patients already received daratumumab for ≥6 cycles and 12 patients were new on daratumumab. Patients already on treatment were followed for 7 cycles with two of three treatments given by a district nurse at home or in a local healthcare clinic, due to differences in the municipal healthcare. Patients new on treatment were followed for 6 cycles with every second treatment given outside the hospital. Prior to each treatment, patients reported their side effects electronically and an algorithm was developed to stratify patients as ready or not for planned treatment. For comparison, patients also had a telephone consultation with a specialized nurse. Patients registered any unplanned contact to the healthcare system between administrations.
Results: In total, 255 of 269 planned administrations of daratumumab were given. All administrations were given safely, no unforeseen events occurred. Of 125 hospital-planned administrations, 122 (97.6%) were given and one was cancelled. Of 144 outsource administrations, 133 (92.4%) were given as planned, six were redirected and given at the hospital (two due to suspicion of infection and four for administrative reasons), and five administrations were cancelled.
On average, patients saved 177 minutes per administration given at home compared to the hospital; 29 vs. 206. Even deducting transportation, time spent was reduced by a factor 3.5 (29 vs. 102). For patients treated at a local healthcare clinic, time was reduced by a factor 3.25 (63 vs. 205). There was no significant difference between numbers of unplanned health contacts between home and hospital administrations. 84% of the patients preferred to continue with home treatment. The PRO questionaries had a positive predictive value of 100%. In no cases did the algorithm recommend treatment when the nurse suggested further medical evaluation. In 171 of 223 questionnaires the algorithm recommended treatment. In 52 cases it recommended medical evaluation. Of these, 44 received planned treatment and 8 were cancelled/postponed. Only 40% preferred to receive calls from the nurse prior to each treatment afterwards. 52 % would like to continue reporting side effects via the app.
Conclusions: Administration of daratumumab by a district nurse is safe, feasible, timesaving, and preferred by the patients. PRO data can effectively evaluate patients prior to treatment.
Methods: From April 2022 to June 2023, 30 patient were included, mean age was 76; range 61-87. Eighteen patients already received daratumumab for ≥6 cycles and 12 patients were new on daratumumab. Patients already on treatment were followed for 7 cycles with two of three treatments given by a district nurse at home or in a local healthcare clinic, due to differences in the municipal healthcare. Patients new on treatment were followed for 6 cycles with every second treatment given outside the hospital. Prior to each treatment, patients reported their side effects electronically and an algorithm was developed to stratify patients as ready or not for planned treatment. For comparison, patients also had a telephone consultation with a specialized nurse. Patients registered any unplanned contact to the healthcare system between administrations.
Results: In total, 255 of 269 planned administrations of daratumumab were given. All administrations were given safely, no unforeseen events occurred. Of 125 hospital-planned administrations, 122 (97.6%) were given and one was cancelled. Of 144 outsource administrations, 133 (92.4%) were given as planned, six were redirected and given at the hospital (two due to suspicion of infection and four for administrative reasons), and five administrations were cancelled.
On average, patients saved 177 minutes per administration given at home compared to the hospital; 29 vs. 206. Even deducting transportation, time spent was reduced by a factor 3.5 (29 vs. 102). For patients treated at a local healthcare clinic, time was reduced by a factor 3.25 (63 vs. 205). There was no significant difference between numbers of unplanned health contacts between home and hospital administrations. 84% of the patients preferred to continue with home treatment. The PRO questionaries had a positive predictive value of 100%. In no cases did the algorithm recommend treatment when the nurse suggested further medical evaluation. In 171 of 223 questionnaires the algorithm recommended treatment. In 52 cases it recommended medical evaluation. Of these, 44 received planned treatment and 8 were cancelled/postponed. Only 40% preferred to receive calls from the nurse prior to each treatment afterwards. 52 % would like to continue reporting side effects via the app.
Conclusions: Administration of daratumumab by a district nurse is safe, feasible, timesaving, and preferred by the patients. PRO data can effectively evaluate patients prior to treatment.