Myeloma Novel Drug Targets and agents
Targeting HVEM using a monoclonal antibody shows therapeutic promise in multiple myeloma
P-275: Targeting HVEM using a monoclonal antibody shows therapeutic promise in multiple myeloma
Wednesday, September 25, 2024

Milad Moloudizargari, DVM PhD
Postdoctoral Fellow
City of Hope
Duarte, California, United States
Introduction: Identifying novel targetable molecules in relapsing patients is an unmet clinical need in multiple myeloma (MM). We previously reported that the oncolytic herpes simplex virus 1 (HSV-1) can infect and kill MM cells via binding to HVEM (TNFRSF14) expressed on MM cells. HVEM is also present on different immune cells and, along with several other ligands, mainly, B- and T-lymphocyte attenuator (BTLA), plays a pivotal immunomodulatory role by regulating T cell activation. We also showed that the expression of HVEM increased on the T cells of multi-relapsing patients and that silencing HVEM in MM cell lines decreased their growth. Building on these findings, we decided to therapeutically target HVEM in MM.
Methods: Human MM cell lines and MM patient samples were studied for their HVEM expression using flow cytometry and gene expressing profiling of datasets that include large cohorts of newly diagnosed MM patients (MMRF CoMMpass Study). Different unique anti-human HVEM monoclonal antibodies (mAbs) were generated and based on their sequence, some were selected to produce murine-human chimeric mAbs. In vitro and in vivo functional studies led us to the selection of a final candidate (aHVEM17), which was fully humanized for subsequent experiments. The tissue specificity of aHVEM17 was studied in healthy and tumor human tissues using imaging mass cytometry (IMC). The anti-MM effect of aHVEM17 was then studied both in vitro and in vivo.
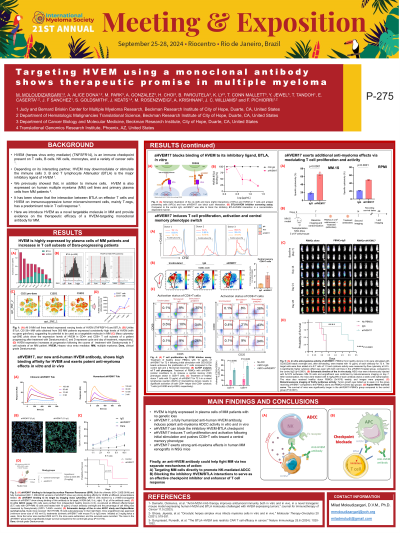
Results: While MM cell lines showed varying levels of expression, HVEM was consistently highly expressed on CD138+ cells of all the studied MM samples without showing any genetic gain and loss. Among the anti-HVEM mAbs generated, aHVEM17 had a high binding affinity (KD= 1.30E-08 M). aHVEM17 binding was specific to BM as evidenced by IMC. In vitro ADCC experiments using MM.1S showed potent ADCC activity of aHVEM17 (10 µg/mL) against healthy donor (HD) NK cells (p=0.0046), which was comparable to that of the standard-of-care Daratumumab (Dara) (p=0.0024). In vivo experiments in nude mice (locally engrafted) and NSG mice (intravenously engrafted) with MM.1S cells showed that the i.v. injection (b.i.w.) of aHVEM17 (5 mg/kg) was able to significantly increase the median survival time from 15 days to 22 days in nude mice (p=0.0147) and from 31 days to 49 days (p< 0.0001) in NSG mice, compared to control IgG. aHVEM17 showed an advantage over Dara as evidenced by significantly less fratricide in NK cells at 24 and 48 h of treatment (10 mg/mL) (p< 0.0001 and p=0.0016, respectively). Furthermore, a HVEM: BTLA inhibitor screening assay revealed that aHVEM17 can block such interaction in a concentration-dependent manner.
Conclusions: aHVEM17 is the first humanized mAb against HVEM capable of inducing potent anti-MM effects thorough NK-mediated ADCC. We are currently evaluating the activity of HVEM, alone or in combination with CAR-T cells, as a possible checkpoint inhibitor for the treatment of MM, the results of which will be presented at the meeting.
Methods: Human MM cell lines and MM patient samples were studied for their HVEM expression using flow cytometry and gene expressing profiling of datasets that include large cohorts of newly diagnosed MM patients (MMRF CoMMpass Study). Different unique anti-human HVEM monoclonal antibodies (mAbs) were generated and based on their sequence, some were selected to produce murine-human chimeric mAbs. In vitro and in vivo functional studies led us to the selection of a final candidate (aHVEM17), which was fully humanized for subsequent experiments. The tissue specificity of aHVEM17 was studied in healthy and tumor human tissues using imaging mass cytometry (IMC). The anti-MM effect of aHVEM17 was then studied both in vitro and in vivo.
Results: While MM cell lines showed varying levels of expression, HVEM was consistently highly expressed on CD138+ cells of all the studied MM samples without showing any genetic gain and loss. Among the anti-HVEM mAbs generated, aHVEM17 had a high binding affinity (KD= 1.30E-08 M). aHVEM17 binding was specific to BM as evidenced by IMC. In vitro ADCC experiments using MM.1S showed potent ADCC activity of aHVEM17 (10 µg/mL) against healthy donor (HD) NK cells (p=0.0046), which was comparable to that of the standard-of-care Daratumumab (Dara) (p=0.0024). In vivo experiments in nude mice (locally engrafted) and NSG mice (intravenously engrafted) with MM.1S cells showed that the i.v. injection (b.i.w.) of aHVEM17 (5 mg/kg) was able to significantly increase the median survival time from 15 days to 22 days in nude mice (p=0.0147) and from 31 days to 49 days (p< 0.0001) in NSG mice, compared to control IgG. aHVEM17 showed an advantage over Dara as evidenced by significantly less fratricide in NK cells at 24 and 48 h of treatment (10 mg/mL) (p< 0.0001 and p=0.0016, respectively). Furthermore, a HVEM: BTLA inhibitor screening assay revealed that aHVEM17 can block such interaction in a concentration-dependent manner.
Conclusions: aHVEM17 is the first humanized mAb against HVEM capable of inducing potent anti-MM effects thorough NK-mediated ADCC. We are currently evaluating the activity of HVEM, alone or in combination with CAR-T cells, as a possible checkpoint inhibitor for the treatment of MM, the results of which will be presented at the meeting.